Get In Touch
Fill out the form below and we'll get back to you as soon as possible.
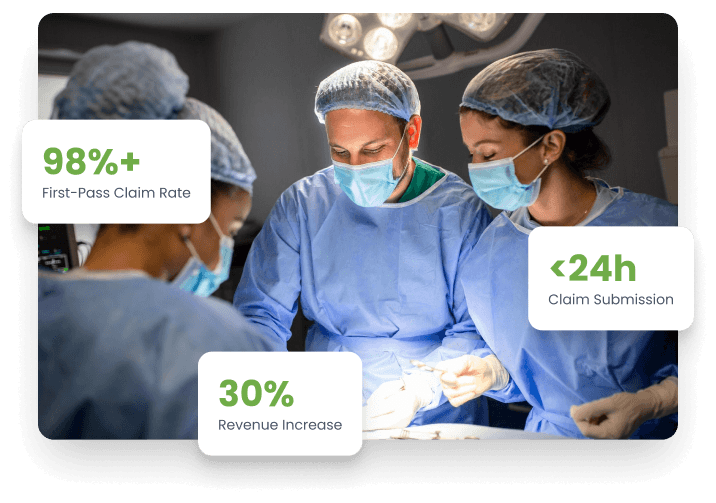
ProMantra has delivered specialized general surgery billing services for over 23 years, helping practices of every size recover more revenue, reduce denials, and reclaim administrative time. Our team of AAPC-certified coders and billing specialists understands the full complexity of general surgery from straightforward hernia repairs to multi-stage trauma reconstructions and translates every procedure into accurate, compliant claims that get paid the first time. As a HIPAA-compliant organization, we operate with the highest standards of data security and regulatory integrity, giving you complete confidence in every aspect of your revenue cycle.
Unlike generalist billing companies that treat all specialties the same, ProMantra’s general surgery billing team brings deep, specialty-specific expertise that directly impacts your bottom line. We stay ahead of annual CPT and ICD-10 updates, modifier rules, and payer-specific policies that are unique to surgical billing. Our coders know the difference between laparoscopic and open approaches, understand when unbundling is compliant, and apply correct global period rules without prompting. That domain expertise is what separates ProMantra from any generalist RCM vendor and why 500+ practices across the USA trust us to protect their revenue every day.
Over 23 years of dedicated general surgery revenue cycle experience
All coding staff hold active AAPC professional certifications in surgical coding
General surgery providers of every size nationwide
Consistently outperforming the industry average of 5–10%
Fully encrypted, and secure at every touchpoint
Our general surgery billing services cover the complete spectrum of procedures performed by general surgeons across hospital, outpatient, and ambulatory surgical center settings.






ProMantra’s general surgery billing services cover the entire revenue cycle from the moment a patient schedules surgery to the final dollar collected. Here is what our team delivers for every surgical practice we serve.

We confirm active coverage, deductibles, co-pays, and out-of-pocket balances before every surgical case so you never perform a procedure without knowing how it will be reimbursed. Our pre-authorization team coordinates benefit checks across all commercial and government payer types.

Complex surgical procedures often require advance approval. Our team manages the full prior authorization workflow like submitting clinical documentation, following up with payers, and escalating peer-to-peer reviews. So your surgeons can proceed without administrative delays or last-minute surprises.
Our AAPC-certified coders assign accurate CPT, ICD-10, and HCPCS codes for every procedure, applying correct modifiers (e.g., -22, -51, -59, -62, -80) and complying with payer-specific bundling rules. Precise coding is the single most impactful factor in achieving a high first-pass acceptance rate.

We capture all billable services from operative notes, anesthesia records, and facility documentation, ensuring nothing is missed. Our charge review process cross-references CDM entries with clinical documentation to catch under-coded or missed charges before submission.

Every claim undergoes a multi-point scrub before submission like checking patient demographics, payer-specific rules, modifier usage, and code pairing. So claims leave clean and arrive compliant within our <24-hour submission turnaround.

Our team posts ERAs, EOBs, and manual payments with same-day accuracy, identifying underpayments and contractual adjustments and flagging discrepancies for immediate follow-up. Accurate payment posting is the foundation of a reliable AR picture.

With a <2% denial rate, we stop most denials before they happen. When denials do occur, our team investigates root causes, corrects errors, and files clinically supported appeals with complete documentation to recover every dollar owed within payer deadlines.

Our AR specialists work aging buckets systematically by prioritizing high-value claims and escalating stalled accounts to keep your days-in-AR low and your cash flow predictable. We pursue every outstanding balance with persistence and professionalism.

Our credentialing specialists manage new provider enrollment, re-credentialing, and payer contract updates so your surgeons are always in-network, billable, and reimbursed at contracted rates without gaps in coverage that interrupt cash flow.

ProMantra delivers customized financial dashboards and monthly performance reports covering collections rate, denial trends, days-in-AR, payer mix, and revenue by procedure giving practice administrators the data-driven insights needed to make informed decisions.
General surgery billing is among the most complex in all of medicine. Between multi-procedure operative cases, global surgery periods, modifier disputes, and payer-specific bundling edits, revenue leakage is common and costly. ProMantra’s general surgery billing services are purpose-built to address each of these challenges at the root level, protecting your revenue before claims ever reach a payer.
General surgery procedures carry 0-, 10-, or 90-day global periods during which related E&M visits and minor procedures may not be separately billable. Incorrect billing within the global period results in denied or recouped claims. Our coders rigorously track global periods and apply appropriate modifiers when separate billing is justified, protecting your revenue and your compliance record.
Modifiers such as -22 (increased procedural complexity), -51 (multiple procedures), -59 (distinct procedural service), and -62 (co-surgery) are frequently misapplied or omitted in general surgery billing. Incorrect modifier usage leads to claim rejections, reduced reimbursements, or audit exposure. ProMantra's coders apply modifiers with surgical precision, supporting every non-standard usage with clinical documentation.
Insufficient documentation is the leading cause of medical necessity denials for surgical procedures. When operative notes fail to capture complexity, diagnosis specificity, or technique used, payers downcode or deny. Our clinical documentation improvement (CDI) process flags incomplete notes pre-submission and works directly with surgeons' staff to obtain necessary addenda before claims go out.
CCI (Correct Coding Initiative) edits govern which surgical CPT codes can be billed together. Improper unbundling triggers automatic denials and potential fraud flags, while over-bundling leaves legitimate revenue uncaptured. ProMantra's billing team cross-references every multi-procedure claim against the CCI table, applying the correct modifier when unbundling is medically justified.
Each major payer like Medicare, Medicaid, BCBS, Aetna, UnitedHealthcare maintains unique coverage policies and LCD/NCD determinations for surgical procedures. What is reimbursable under one plan may be denied under another. Our team maintains current payer policy libraries and verifies coverage criteria before submission, dramatically reducing preventable denials.
Surgeons operating in both hospital outpatient departments (HOPD) and ambulatory surgical centers (ASC) must bill under facility-specific fee schedules and rules. Applying the wrong place-of-service code or OPPS rates to ASC cases generates significant payment errors. ProMantra manages facility-type billing correctly across every setting your surgeons use, ensuring accurate reimbursement every time.
ProMantra’s structured 8-step process ensures that every general surgery claim is handled with precision from pre-service through final payment by eliminating gaps that cost practices thousands in lost revenue.

We verify insurance eligibility and obtain required prior authorizations before each scheduled surgical case, eliminating coverage-related surprises and ensuring every procedure can be billed as intended.

Our team reviews the operative note, anesthesia record, pathology reports, and discharge documentation for completeness and medical necessity before a single code is assigned.

AAPC-certified coders assign all CPT, ICD-10, and HCPCS codes, applying modifiers per CMS, AMA, and payer-specific guidelines. Complex multi-procedure cases receive a second-level review for accuracy.

We reconcile all billable charges from the surgical case against the practice management system to identify missing charges, duplicate entries, or documentation-coding mismatches before submission.

Every claim is run through our multi-rule scrubber from checking patient data, payer edits, code pairing, and modifier logic to ensure zero clean-claim errors leave our system.

Clean claims are submitted electronically to the payer within 24 hours of encounter finalization, maximizing cash flow velocity and meeting all timely filing requirements.

Payments are posted daily, with ERA/EOB reconciliation identifying contractual adjustments, underpayments, and patient responsibility transfers in real time.

Denied claims are worked within 24–48 hours of receipt. Our AR team pursues all aging claims systematically, and monthly reports give you complete financial visibility.
Accurate coding is the engine of every successful general surgery billing services engagement. ProMantra’s coders bring specialty-depth expertise across every dimension of surgical coding.
Our coders are fluent in the 10000–69999 surgical CPT code range, with deep specialization in 40000–49999 (digestive system), 19000–19499 (breast), and 60000–60699 (endocrine system) subsections.
We select the highest-specificity ICD-10 codes to support medical necessity and minimize payer scrutiny, including correct laterality, etiology, complication coding, and postoperative status.
Our team correctly applies 25+ surgical modifiers including -22, -51, -52, -53, -59, -62, -66, -78, -79, -80 with supporting documentation that withstands payer audit review.
Every claim is cross-referenced against the CMS National Correct Coding Initiative (NCCI) edits to prevent unbundling errors and confirm compliant code pairs before submission.
We maintain real-time global period logs by patient and surgeon to ensure correct billing of E&M visits, return surgeries, and related procedures within and outside the global window.
Our coders accurately split professional and facility components and apply the correct fee schedule like HOPD, ASC, or inpatient for every case setting where your surgeons operate.
We understand how general surgery procedures interact with anesthesia billing (base units, time units, qualifying circumstances), preventing conflicts between surgeon and anesthesia claims.
Our team correctly codes pre-operative consultations, intraoperative decision-making, and post-operative E&M visits to capture every billable encounter within regulatory guidelines.
At ProMantra, we don't ask you to take our word for it, we show you the numbers. Here is what general surgery practices consistently experience when they move their billing to ProMantra:
First-pass clean claim rate. Compared to the industry average of 75–85%

Average revenue increase for new clients within the first year

Average turnaround from charge capture to payer receipt

Average Days in AR. Compared to the industry average of 50–60 days

Overall denial rate. Compared to the general surgery industry average of 5–10%

First-level appeal success rate

Surgical practices served nationwide

In healthcare revenue managed annually across all specialties

These numbers are not projections, they are averages drawn from active client results. When you choose ProMantra as your general surgery billing partner, you are choosing a company that has consistently delivered measurable, documented results for practices just like yours across every region of the United States.
When our two-surgeon general surgery practice transitioned to ProMantra, we were sitting on over $400,000 in denied and aging AR. Within six months, ProMantra's team had recovered $380,000 through systematic denial appeals and payer follow-up. Our first-pass acceptance rate jumped from 82% to 97%, and our days-in-AR dropped from 68 to 31. We finally have a billing partner that understands surgical coding at the level we need.
We had been using a regional billing company that did not specialize in surgery. Modifier errors and unbundling mistakes were costing us thousands every month. Since switching to ProMantra's general surgery billing services, our collections increased 34% in the first quarter and our denial rate is now under 2%. Their coding team knows surgical billing inside and out, it shows in every EOB we receive.
As we expanded from one to four surgeons, our in-house billing team could not keep up with the volume or complexity of our cases. ProMantra stepped in seamlessly, handling credentialing for our three new providers, managing a complex payer mix, and driving our clean claim rate above 98%. Their reporting dashboard gives us exactly the financial visibility we need to run the business side of our practice.
See how we’ve helped healthcare organizations like yours achieve measurable revenue growth

Multi-Specialty Hospital
Download Case Study
Please fill out the form below to download the case study.

Surgery Centre
Download Case Study
Please fill out the form below to download the case study.

Surgical Centre with Lab Services
Download Case Study
Please fill out the form below to download the case study.
ProMantra’s general surgery billing services are designed for every practice model and setting that general surgeons operate in across the USA.
Making the decision to outsource your general surgery billing is a significant step and we understand that uncertainty about the transition process is one of the biggest barriers practices face. That is why ProMantra has built a seamless, structured onboarding experience that gets your billing live within 7 to 14 business days without disrupting a single patient encounter.

We start with a thorough practice assessment by reviewing your current billing workflows, payer mix, fee schedules, coding history and EHR or practice management system. Our integration team connects with your existing technology environment, and a dedicated account manager is assigned to your practice immediately.

Your billing team is fully configured. We establish escalation protocols, reporting schedules, authorization workflows, and coding preferences specific to your practice. You receive direct contact information for your account manager and can reach them by phone or email during business hours.

Your claims are live. Our team is submitting charges, posting payments, and managing denials with complete transparency through your real-time client portal. You will see exactly what has been submitted, what has been paid, and what is in follow-up at any moment.

We analyze early data to identify coding gaps, undercoding patterns, payer trends, and denial root causes. Adjustments are made proactively to optimize your clean claim rate and collections, not reactively after problems compound.

Quarterly business reviews, continuous compliance monitoring, payer policy updates, annual CPT and ICD-10 training, and dedicated support ensure your revenue cycle stays optimized year after year. There are no surprises, no hidden fees, and no long-term lock-in contracts.

A detailed 90-day review with your account manager highlights the improvements in revenue, AR days, denial rates, and collections efficiency. Most ProMantra clients report a 20–30% improvement in net collections by this milestone.
Discover how much revenue you’re leaving on the table. Our experts will analyze your current billing performance and provide a detailed improvement plan at no cost.








Need a custom RCM solution?
Outsourcing your revenue cycle to a specialized partner is not an expense, it is one of the highest-return investments a surgical practice can make. ProMantra’s general surgery billing services eliminate the cost and risk of maintaining an in-house billing department while delivering measurably better financial outcomes. Our clients consistently report a 30% or greater increase in collections within the first 90 days, driven by reduced denials, faster claim submission, and comprehensive AR recovery that leaves no revenue on the table.
When you partner with ProMantra, you gain a full team of AAPC-certified coders, AR specialists, credentialing experts, and reporting analysts without adding a single line item to your payroll. We work as an extension of your practice, aligning our performance goals with your revenue targets and providing complete transparency through real-time dashboards and monthly executive reports.
Most practices are fully onboarded within 7–14 business days. Our implementation team handles data migration, payer setup, and workflow integration with minimal disruption to your daily operations.
Yes. We manage professional fee billing, ASC facility billing, and hospital outpatient billing by applying the correct fee schedule and coding guidelines for each setting.
ProMantra offers flexible engagement models. We believe in earning your business through performance, not contracts, and will work with your practice to find the right service arrangement.
When you partner with ProMantra, you get three outcomes that directly impact your practice’s future: MORE REVENUE COLLECTED, FEWER DENIED CLAIMS, and COMPLETE PEACE OF MIND that your general surgery billing is handled by the most experienced team in the USA.
Connect with Our Team
Submit your details and we’ll reach out to assist you.
Below are the most common questions practice administrators and surgeons ask when evaluating ProMantra’s general surgery billing services for their practice.
General surgery involves high-complexity, multi-procedure operative cases that require precise CPT code selection, accurate modifier application, and strict adherence to global surgery period rules. Unlike office-based specialties, surgical billing must account for facility type (hospital vs. ASC), anesthesia interaction, CCI bundling edits, and payer-specific coverage policies for each procedure performed. Errors at any stage from documentation to submission can result in significant revenue loss and compliance exposure. ProMantra’s specialized team is trained exclusively on these surgical billing nuances, which is why our general surgery clients achieve a 98%+ first-pass acceptance rate across all payer types.
Our AAPC-certified coders follow a structured review process: they begin with the operative note, pathology reports, and anesthesia records, then assign primary and secondary CPT codes, apply CCI edits, and determine correct modifier usage. For cases involving three or more procedures, a senior coder performs a second-level accuracy review before submission. We also conduct monthly coding audits benchmarked against payer feedback to continuously improve performance. This rigorous process ensures that every complex surgical case is billed completely, compliantly, and at the highest supportable level of reimbursement.
The global surgery period is a defined timeframe like 0, 10, or 90 days depending on the procedure during which certain follow-up services are included in the surgical fee and cannot be billed separately. Billing related E&M visits or minor procedures during the global period without proper modifiers results in denied or recouped claims and potential compliance risk. ProMantra maintains real-time global period tracking for every patient by procedure, automatically flagging claims that fall within the global window and applying the appropriate modifier (such as -24, -25, or -79) when separate billing is clinically and regulatorily justified.
Our prior authorization team submits requests directly to payers through electronic portals and phone follow-up, including all supporting clinical documentation such as operative planning notes and imaging reports. We track authorization status for every scheduled case and alert your clinical staff immediately if approval is delayed or denied. When initial authorizations are denied, we coordinate peer-to-peer review consultations between your surgeon and the payer’s medical reviewer, giving your team the best possible chance of approval for every medically necessary procedure without administrative burden on your staff.
ProMantra maintains a less than 2% overall denial rate across our general surgery client base well below the industry average of 5–10%. When denials do occur, our team responds within 24–48 hours, analyzing the denial reason code, correcting any billing or coding error, and filing a complete appeal with supporting clinical documentation. Our appeal success rate exceeds 90% for overturned claims. Every denial is also tracked for root cause trend analysis, allowing us to address systemic issues and prevent recurrence across your entire claim population going forward.
Absolutely. Many of our general surgery clients operate across hospital outpatient departments, ambulatory surgical centers, and inpatient settings simultaneously. We manage professional fee billing regardless of facility and handle ASC and hospital facility billing where applicable, applying the correct fee schedule, place-of-service code, and billing rules for each setting. Multi-site billing complexity is something ProMantra handles every day for surgical practices nationwide, and our team ensures that the correct claim format and fee schedule are applied every time regardless of where the procedure takes place.
Our coding team undergoes mandatory continuing education and AAPC recertification annually, with specific focus on annual CPT updates from the AMA and ICD-10-CM updates from CMS effective each October 1. We maintain active subscriptions to payer policy bulletins, CMS transmittals, and specialty-specific coding guidance from the American College of Surgeons (ACS). When a significant coding change affects general surgery such as new laparoscopic CPT codes or revised global period rules, our entire team is briefed and updated within days, not months, ensuring your claims always reflect current coding standards.
We deliver comprehensive monthly financial performance reports that include: gross charges and net collections by provider, first-pass acceptance rate, denial rate by payer and reason code, days-in-AR, aging AR breakdown by payer bucket, collections by CPT code, payer mix analysis, and month-over-month trend comparisons. Practices also receive real-time access to a secure performance dashboard for on-demand financial visibility between reporting cycles. These reports are designed to give practice administrators and physician owners the data they need to identify revenue gaps, evaluate payer performance, and make strategic financial decisions.
ProMantra is a fully HIPAA-compliant organization. All patient data is transmitted and stored using AES-256 encryption, and access is controlled through role-based permissions with multi-factor authentication for all team members. We conduct regular internal security audits, mandatory staff privacy training, and third-party security assessments to maintain compliance with the highest data protection standards in the industry. Our Business Associate Agreement (BAA) is provided to every client as part of our standard engagement process, ensuring your practice’s compliance obligations are fully met from day one.
Getting started is simple. Contact our team for a complimentary revenue cycle assessment, during which we evaluate your current collections rate, denial trends, AR aging, and coding accuracy. Based on this analysis, we provide a customized service proposal and transition plan tailored to your practice’s specific needs and volume. Most practices are fully onboarded within 7–14 business days with zero disruption to ongoing claim submission. Our implementation team handles every aspect of the transition, including EHR integration, payer credentialing updates, and staff communication protocols. To schedule your free revenue cycle assessment, visit promantra.us or contact our team today.
Not sure whether your current billing process is leaving revenue on the table? You are probably right to wonder. ProMantra offers a complimentary, no-obligation general surgery billing assessment that gives you a clear, honest picture of your practice’s revenue cycle performance and exactly what we would do to improve it.
There is no obligation and no sales pressure. If you decide ProMantra is not the right fit, you walk away with a free, expert analysis of your revenue cycle and actionable recommendations. If you do choose to partner with us, you start from a position of complete clarity about where your revenue is going and how much we can recover.